Community Corner
The Village That Sophie Built: An Oak Forest Preemie's Story
Katy and Tim Landuyt could talk about their little girl all day. They want her—and their family's story—to remind people they're not alone.

OAK FOREST, IL — Katy Landuyt likes to stay occupied nowadays. The 30-year-old, lifelong Oak Forest resident finds her hands even busier than usual heading into the holidays.
Katy and her husband Tim, 35, will make as many fleece blankets as they can, to hand-deliver to the littlest residents of the Silver Cross Neonatal Intensive Care Unit in New Lenox—where one month ago they said goodbye to their daughter.
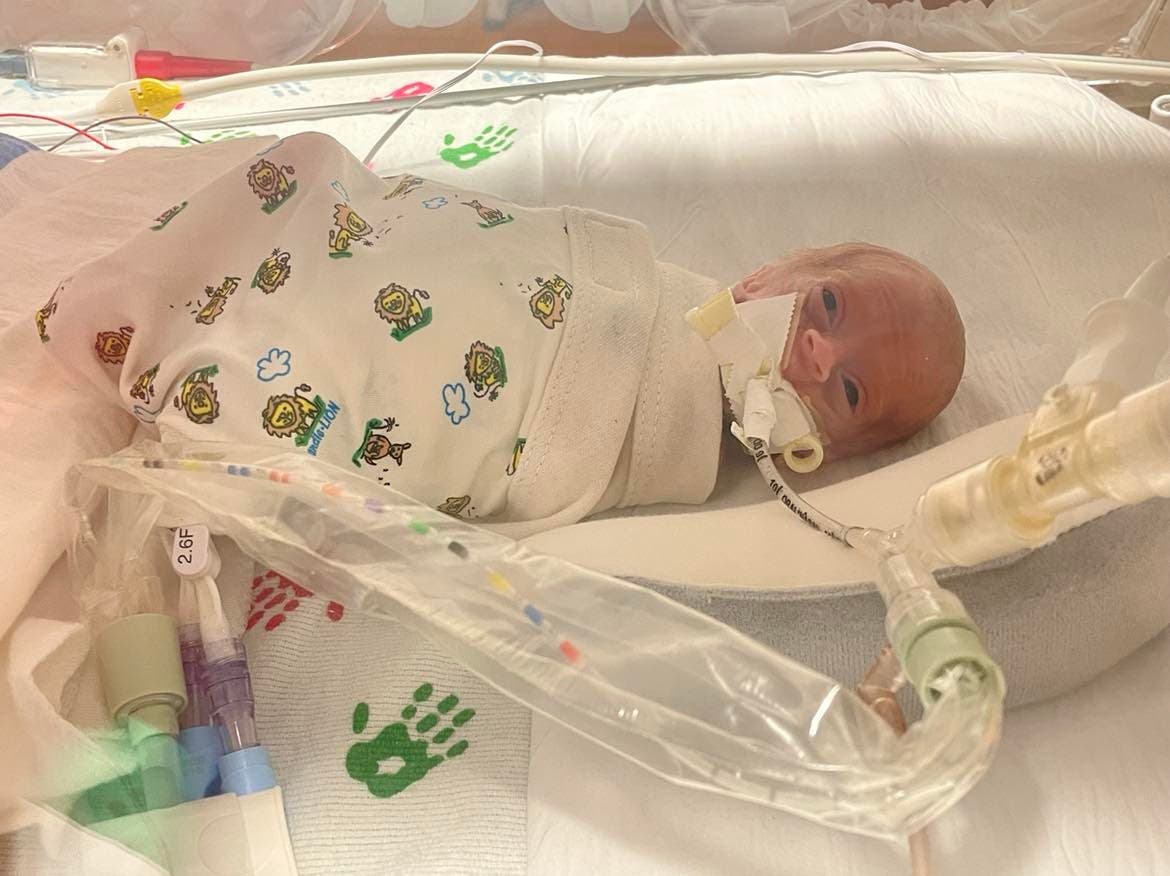
Sophie Jean Landuyt wasn't here long, but you'd never know it by the impact she had on so many. The preemie was born Sept. 16, 2022, weighing just 14 ounces at 24 weeks. From the moment of her birth, her parents knew she—and they—would be in a fight for her life.
Find out what's happening in Oak Forestfor free with the latest updates from Patch.
But the couple was used to putting up a fight for what they want. They knew going into their marriage that building a family would be challenging for them; they didn't expect it to come easily, and they were right. The pair conceived two children, both through extensive in vitro fertilization and medical intervention, a journey they think so many may be afraid to share.
They had fought hard for "Soph" to become part of their family, and they'd fight alongside her as long as she had it in her, Katy said.
Find out what's happening in Oak Forestfor free with the latest updates from Patch.
"We said the whole time that we were going to let Soph drive, from the very beginning," Katy said."We said we felt like we would know if she was giving us a sign. We didn't want to push her too much and then have her struggle in life. ... We felt like if we kept saying that she was going to drive and we were going to listen to her signs, then we would know what to do."
Now one month past their daughter's death, they want to tell their family's story: one of Sophie's too-short stay here, and a village that rallied around her.
A Numbers Game
Katy was 26 years old when she was diagnosed as being in early menopause. Conception would be difficult, but not impossible, and not yet married, she and Tim realized they'd be in it together. Their firstborn Ryne, now 3, was conceived after two IVF cycles with Chicago IVF fertility clinic. The pair had just a 2 to 3 percent chance of conceiving, their doctor told them. The first cycle had been cut short halfway through, Katy said. The second took several weeks of two injections a day—all timed perfectly, sometimes given in peculiar circumstances like at a wedding, or in a bar bathroom, whatever it took to get it done. The process resulted in three eggs, two fertilized. Both were transferred, and they "then got Ryne out of the deal," the two say, smiling.
In their first attempt at a sibling for Ryne, they turned to the same clinic. After seeing zero eggs result from their first retrieval following one cycle, they changed doctors and clinics, instead now turning to Dr. Scott Springer of Vios Fertility (now Kindbody). The use of an egg donor had been suggested, and they went into their meeting knowing that might be their best hope. They even had someone in mind. But their new doctor wasn't so sure he couldn't help them another way.
"We told him all about our story, and he was kind of older school," Katy said. "He wanted to give it one more try."
From their first Zoom meeting, Katy had a feeling about Dr. Springer. He "looked identical" to her father, who had died 7 years earlier, she said.
"I had a good peace, that this was going to work," Katy said. "He was older, we had a good vibe with him right from the start. He loved that we had a donor possibly lined up and in our back pocket, but he wanted to give it one more try with me, and try things the other doctor hadn’t done, some other protocols."
Their likelihood of conceiving had now dwindled down to 1 percent. One cycle yielded three eggs: two matured, and only one fertilized for transfer. It worked; a total of 202 injections later, they finally conceived.
"Kind of weird we had three eggs (for both pregnancies)," Katy said. "... Numbers have really worked out, and have been weird that they've correlated so much."

'You don't even look like you're pregnant!'
Katy realized her second pregnancy was different when people started remarking how very not-pregnant she looked. She had shown so early with Ryne, she said, but she pushed off the worry as long as she could. Her early maternal fetal medicine appointments showed the baby was measuring healthy, but that the ambilical cord was pulling. Katy would be checked again at 32 weeks, her doctor said, to make sure their daughter was still growing as needed, and if not, Katy would be put on bedrest prior to an early delivery.
Another doctor's appointment two weeks later on Sept. 9, Katy was 24 weeks pregnant when she told her doctor she felt like hadn't gained much weight, but her doctor assuaged her fears. The couple then went out of town for the weekend, where Katy noticed swelling in her feet, and a shortness of breath. Suddenly, she was very noticeably swollen in several places, and suddenly very visibly pregnant. Her doctors told her to go to Silver Cross Hospital, where the baby's heartbeat was hard to find at first, and Katy's blood pressure spiked.
She was in the hospital overnight—and the next day was ordered to stay there, on bedrest. Within a day things began moving fast, with numbers and prognoses flying. The umbilical cord was at high risk of rupturing, Katy said, and before she and Tim knew it, an emergency Cesarean section was scheduled.
Katy had delivered Ryne at Northwestern Medicine Palos Hospital, with assistance from staff from Advocate Christ Medical Center. Now at the the recently opened Silver Cross Hospital NICU, some staff from Advocate who had helped deliver Ryne, had also moved to staff the new unit at Silver Cross. That included Dr. Mario Sanchez, who had been in the room for his delivery.
"I was laying there, waiting to be put under, and the neonatal doc came in, and I had complete deja vu," Katy said. "He was the same doctor that was there in the delivery room for Ryne, and he was there for Sophie. ... Totally different hospitals, different situations. ... It was a sense of peace that it was the same doctor."
Hard conversations swirled around Tim as his wife was put under anesthesia. What measures would he want them to take to save their premature daughter or his wife, who also had health complications?
"We could come in here with two people, and you could, in theory, go home with nobody, because of how rapid everything was moving," Tim said doctors told him.
"Whirlwind of emotions isn't even the right way to describe everything that was going through my mind."
The couple had discussed what would happen if Katy's life weighed more heavily in the balance during a difficult delivery.
"Ryne needs me to come home from the hospital," Katy said, of their son needing his mother.
At 24 weeks, their daughter's lungs would not be developed enough for her to breathe on her own; she would need to be intubated, an intricate and challenging procedure at such a small size. Doctors warned there was a chance her throat would be so narrow, even the hospital's smallest tube would not fit.
Tim waited outside during the C-section, and he can remember the moments he held his breath, hoping that each one he skipped would give his daughter another to breathe.
Somewhere in the midst of his bated breath, Sophie was born and successfully intubated, by Dr. Sanchez.
'We're able to give babies a fighting chance'
Back home, Sophie's extended family rallied around her, starting a Facebook group called Sophie Jean Strong to share her progress. Sophie needed their support.
The odds are stacked greatly against babies born at just 24 weeks—with major organs not yet developed enough to sustain them naturally—and every inch of Sophie's tiny body was in battle.
"Every organ system that the baby relies upon is underdeveloped at that time," said Dr. Brett Galley, of Silver Cross Hospital's Neonatal Intensive Care Unit, and Sophie's doctor. "At 24 weeks, the lungs are just beginning to develop the air sacs that allow us to exchange oxygen into our blood from the air, so that’s what really puts these babies at a severe disadvantage."
The brain is "far from the point of being fully developed," and unique to premature to babies, there are very fragile blood vessels in the center of the brain that are very prone to rupture, Galley said. That can lead to hemorrhages in the center of the brain that can cause long-term problems. Also among other complications, intestines aren't yet ready to digest, so feeding tubes are required as a source of nourishment.
"At 24 weeks, things are just getting around to the point where the babies have a chance of having us help them out," Galley said.
Advancements in medicine have extended a premature baby's chance of survival, or viability.
"In general, the threshold of viability 10 to 15 years ago was 24 weeks," Galley said. "It’s moved to about 22-23 weeks, because we’re able to give the babies a fighting chance. But it’s still a difficult road for these babies, because there are so many things we need to do, to be able to help them sustain themselves until their organ systems can."
Sophie was no exception. Born on a Friday, it seemed that each subsequent Friday brought about a new twist. On the second one, she was airlifted to Lurie Children's Hospital in Chicago, after having sudden drops in heart rate, and needing a new PICC line—or percutaneously inserted central catheter—to help provide her nutrition. The line would have to be inserted surgically at Lurie. The couple watched as a helicopter carried their daughter to the next hospital.
"Neither one of us thought that she was going to be alive when we got there," Katy said.

'Good' Fridays from now on'
After a week at Lurie, Sophie was stable enough to be transported back to Silver Cross, where familiar faces awaited her and her exhausted parents.
Talking about it now, Katy and Tim lock eyes as if they're seeing it play out in real time; two who fought alongside each other and their daughter, now recounting each moment good and bad, seeing it through the other's lens.
The return to Silver Cross was a "good" moment.
"That was our turn, we're going to have 'good' Fridays from now on," Katy said they thought to themselves.
Katy and Tim had grown close to several members of the nursing staff—Jenna H., Shell K., Kaity B. and Amy S.— and going back to Silver Cross gave them a sense of going "home." The staff had formed a village around Sophie, giving the couple constant updates on her condition, sharing significant and touching moments of their daughter's days. The staff became like family, sharing in milestones and setbacks. Katy and Tim felt certain Sophie was getting the most attention there.
"At Silver Cross, she was the sickest baby," Katy said, "... I want her to be at the hospital that's showing her the most attention, and is the most hands-on, and are most nervous about it, because they're going to be giving her all of their attention."
Worries of a blood infection and problems with her lungs kept her parents fraught with worry throughout the week. Then came isolation for MRSA and a staff infection.
"When they say that living the NICU lfe is a rollercoaster, it's the most extreme rollercoaster I've ever been on," Katy said. "Some days were so good, I would leave feeling so great, and then some days I would think we should start making arrangements."
One day they brought Ryne up to meet his baby sister, and the siblings put on Halloween costumes for a quick photo.

"She was super-alert," Katy said.
"She knew something was going on, she wanted to be a part of it," Tim said.
A blood infection then took its toll on Sophie, and she was moved back to the ventilator she had been put on at birth—a regression of sorts, doctors said.
The couple always asked Dr. Corryn Greenwood not to sugarcoat things for them, and that day, they remember hearing what they'd been dreading:
I haven't been worried, but I'm really, really worried about Soph now.
— Dr. Corryn Greenwood, Silver Cross NICU
As Sophie's oxygen level hovered low at 60 percent, doctors urged Katy to put her hands on her.
"The second I did that, her oxygen spiked to 80 percent," Katy said.

It didn't last long before her oxygen dropped again and the staff turned to CPR. It was the first time they thought she might be done fighting.
With hope dwindling, the staff prepared to let Tim hold his daughter for the first time. He and Katy then held her together, and a priest from St. Damian arrived to baptize her. Family waited outside the building, praying.
Sophie was born at 2:40 a.m., Sept. 16; she died at 2:40 p.m. Oct. 16., just 12 hours past a month since she had been born.
'That's not how it should be'
The medical staff was almost just as rocked by Sophie's death as her parents. The couple struggled with the steps following her passing, like the hospital's insistence that their child's body be taken to the morgue. They called the funeral home and asked for a bedside pick-up.
"No parent should take their NICU baby off of life support and be told she has to go to the morgue," Katy said.
They wonder if it's a procedure they might be able to help change, Katy said. It's something they want to work on for future parents facing the same situation.
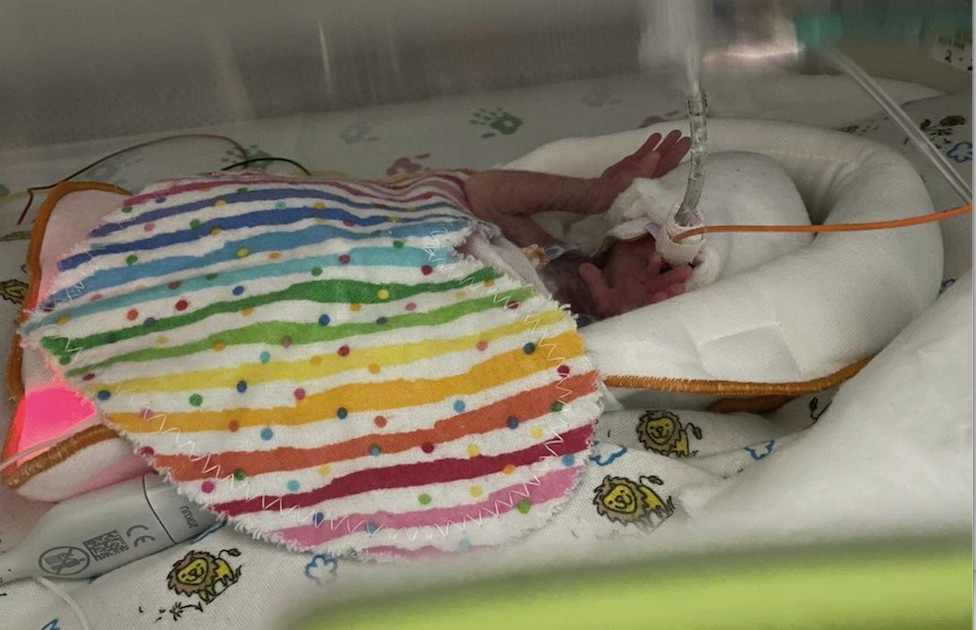
They had noticed other ways they might help the Silver Cross NICU, too. As a newer unit, it lacks some of the community donations from which others benefit, such as items known as "bonding hearts."
"Bonding hearts" are heart-shaped swaths of fabric, preferrably flannel, that mothers are encouraged to place against their bare skin, to then be laid over the infants in their mother's absence, and vice versa. The fabric exchanges scents between mother and baby, helping to aid the mother in production of breast milk, and comfort the infant in the mother's absence.
"The baby then can get the sense that mom’s nearby," Galley said, which often shows up in physiological ways such as stabilized vitals and increased oxygenation levels.
The parents' proximity to their infants—while often difficult to arrange—is crucial to helping the infants improve, he said.
"That gets very challenging as these babies are very sick and unstable," Galley said. "Finding ways of families to be at the bedside, and to provide that touch is really very important. Sometimes we do have to get creative."
Other comfort items can be provided by community members. Handmade, donated blankets are used to drape over the isolettes the babies spend so much time in, Galley said.
".... we’ve done a lot of work to make the NICU rooms very welcoming and warm environments for the families in order to promote their wellbeing when they’re there," Galley said. "Those personal touches are really important, to make the space their own. To have those kinds of things that aren’t medically provided, is really important for families to feel at home, and to feel some sense of normalcy."
Experience has shown Katy and Tim that he's right, and they're focusing on collecting items for donation to the Silver Cross NICU. In addition to monetary donations to the Sophie Jean Strong GoFundMe—to be used to purchase supplies for the unit—Katy and Tim have placed dropboxes at locations in Oak Forest for anyone who would like to donate handmade fleece blankets or bonding hearts.
Bonding hearts should be about 7 inches by 6 inches, Katy said, and preferably made of flannel. Blankets should be two pieces of fleece measured 36-inch by 28-inch laid atop each other, with 1.25-inch wide stips cut to be about 4 inches long, around all four sides. Those strips are then tied into knots.

"Sophie was with us on Earth one month and it’s been one month without her," Katy wrote on the Sophie Jean Strong Facebook page, as her family made blankets in her honor Nov. 16. "Today, we make NICU blankets as a family and pray for the other families who will be faced with a NICU stay."
Galley said such small touches—or items that simluate connection—can have a huge impact on the babies in the NICU.
"At the beginning of the advent of neonatal were put in isolettes, and no one touched them but nurses," Galley said, "And rightfully so. Everyone was concerned about how fragile these babies are.
"Touch by mothers and fathers is really crucial, not just for bonding, but physiologically these babies become more stable."
Some parents of babies born at Sophie's stage don't get much time with them, and Katy think that's also what's made memories of Sophie stick with the staff.
"So many babies that are less than a pound don't make it out of the delivery room," Katy said.
"Even though she never left the hospital, she had a pretty good quality of life. She had a lot of friends ... she's brought a lot of people closer together.
"She's brought us closer together," Katy said, of herself and Tim.
Their hometown community also stepped up for them, a "serious village" arranging Amazon packages dropped at their doorsteps.
"We had books delivered daily (we read to Sophie daily as studies show reading to them helps," Katy said. "We asked people to wear green for NICU awareness week and even Rynes class got wind of it and wore green. It was overwhelmingly beautiful.
"It's just crazy how many people flock back when there's a time of need."
They want families who endure IVF to know they're not alone in their struggle.
"Some people are lucky enough to have kids ... it just happens, unfortunately there are a lot of people who try so hard just to have one," Tim said.
The couple will not seek to conceive again, but will always consider themselves a family of four.
"We're always going to say Sophie's name in our family," Tim said. "It's not just Katy, Tim and Ryne. It's Katy, Tim, Ryne and Soph. It's always going to be the four of us."
Tim said he's grateful to the Silver Cross staff who held Sophie and their family so close during her short time at the unit.
"I owe so much gratitude to these people," Tim said. "Sure, did it end the way we wanted it to? No, but that's not their fault. These people are taking the hardest time for some people in their lives, and they treat them like they're their own kids.
"Gratitude's probably not even the right word."
Through Jan. 6, 2023—Sophie's original due date—Katy and Tim will collect donations of fleece blankets and bonding hearts at the Oak Forest Park District, 15601 Central Ave., and Oak Forest City Hall, 15440 Central Ave.
Anyone needing more information should email sophiejeanstrong@gmail.com.
November 17 is known as World Prematurity Day, to raise awareness of premature births and the sometimes devastating impacts on families. An estimated 15 million babies worldwide are born premature each year, according to the World Health Organization. The CDC reports that in the United States in 2021, one of every 10 infants was born premature.

Get more local news delivered straight to your inbox. Sign up for free Patch newsletters and alerts.