Crime & Safety
Curbing Opiates: Doctors Addicted To Overprescribing
Many people's battles with addiction begins in a doctor's office. Now officials are looking to curb the overprescribing of opiates.

BEREA, OH - Nicole Walmsley’s trip into addiction, like so many others, started because of a thoughtless prescription given to her by a doctor. She was in her early 20s, between 2006 and 2007 she says, and had just been diagnosed with endometriosis. She underwent back-to-back surgeries for her condition and her physicians prescribed her a potent pain pill.
The problem was, Walmsley had a family history of drug addiction. In fact, her mother was a drug addict and when Walmsley was born in Akron, she had drugs in her system, she says. While Walmsley’s adoptive family chose not to share that information with her, they shared her background with the doctor. He prescribed the pain pill anyway.
“The doctor knew I had a predisposition to addiction but did not educate me on what this pill was. I thought, ‘He’s got a white coat and a degree, he knows what’s best for me,’ ” she says looking back on the situation.
Find out what's happening in Middleburg Heights-Bereafor free with the latest updates from Patch.
Once she popped that first pill, her life instantly changed forever.
“It changed something in me chemically. Everything that I felt was wrong was fixed by this one pill. Then I abused it. I started snorting it,” she says. “When I was taken off it, I was getting sick and I didn’t know why. Then my friend said, ‘You’re dope sick.’ ”
Find out what's happening in Middleburg Heights-Bereafor free with the latest updates from Patch.
(This is part two of a two part series. To read part one, click here.)
That same friend offered to get Walmsley help. Of course, his help came in the form of oxycodone.
She took the oxy. She justified it to herself, saying things like, “Well, I was already prescribed pain pills, so taking these makes sense.”
While she was snorting oxycodone, she swore she would never touch heroin. Heroin was beneath her.
“I had convinced myself that I was still classy because I was snorting oxy. That’s the insanity of addiction,” she says.
Classy or not, she still needed her oxycodone fix. One day she waited five hours for her drug dealer. She was starting to get dope sick, and she thinks her dealer may have known that. When he finally showed up, he told her he didn’t have any oxy.
But he did have a $50 bag of heroin. Maybe she’d like that instead?
She argued. She wasn’t that person, she’s not like that, she said.
So her dealer sweetened the pot. Buy the heroin, use it to get through the night, and he’d hook her up with two pills the next day for her troubles.
“I was thinking, ‘Oh my God, he cares about me,’ ” she says, now mocking her old self.
“I took that bag and never went back to oxy,” she says. “I was paying $50 for a pill, and a $50 bag of heroin lasted me almost a day and a half. Why would I go back? I was still classy, because I was snorting, I was just now doing heroin.”
But the snorting high didn’t last long either. She started to build up a tolerance and was snorting more and more to get through the day. Finally, one of her friends asked her why she didn’t just shoot up?
“I was reluctant at first, but when I shot up the first time I sold my soul. I sold everything I was. I basically married heroin. That was it,” she says.
Since that day, she racked up a long rap sheet that includes a pair of felonies and an overdose.
She’s clean now, and an advocate for the Police Assisted Addiction and Recovery Initiative (PAARI) in Ohio and a national outreach coordinator and law enforcement liaison for Satori Waters, a rehab facility in Florida.
“I do think a lot of people go into their addiction not knowing what they’re going into. People take a pain pill that was prescribed to them, they want to cover up a physical pain, and then it covers up another, deeper pain and they’re addicted,” she says.
The state of Ohio, and the US government, have noted that many addiction stories seem to start the same way: An unsuspecting person goes into a medical facility and gets prescribed an opioid, and boom, an addict is made. In fact, U.S. Sen. Dianne Feinstein, a California Democrat, pointed out a study from Substance Abuse and Mental Health Services Administration that found four of every five heroin abusers also abused prescription drugs in the past.
Curbing Over-Prescribing
The U.S. Centers for Disease Control and Prevention say the sale of prescription opioids quadrupled in the United States between 1994 and 2014. Yet, the agencies say, there has not been a corresponding increase in Americans reporting pain.
The CDC thinks the problem of opioid addiction is rampant and medical professionals bear at least some of the blame. The agencies cite a 2010 study that found one out of every five patients in an office-medical setting is prescribed an opioid.
Dr. Nora Vaklow, director of the National Institute on Drug Abuse (NIDA) at the National Institutes of Health, offered an explanation of the exponential growth in opioid use in a presentation to the Senate Caucus on International Narcotics Control in 2014.
“Several factors are likely to have contributed to the severity of the current prescription drug abuse problem. They include drastic increases in the number of prescriptions written and dispensed, greater social acceptability for using medications for different purposes, and aggressive marketing by pharmaceutical companies,” she said at the time. “These factors together have helped create the broad “environmental availability” of prescription medications in general and opioid analgesics in particular.”
While doctors across the nation may be overly reliant on opioids, Ohio’s medical professionals appear to be particularly keen on prescribing potent opioid-based painkillers. The chart below is from the CDC.
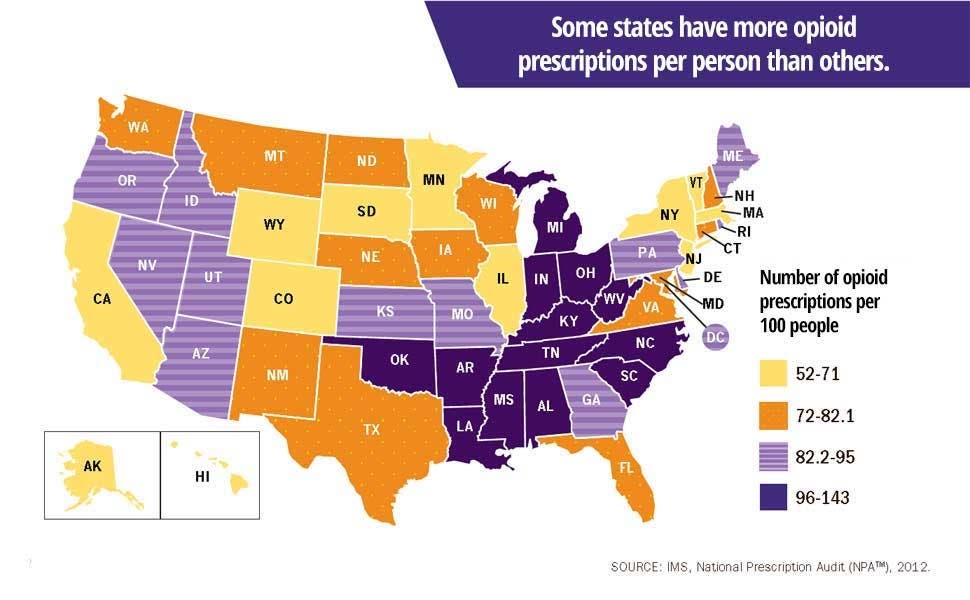
That’s why the state of Ohio is attempting to rein in medical professionals by more tightly regulating the instances in which they can prescribe opioids.
First, Gov. John Kasich issued an order limiting the duration of opioid prescriptions from physicians and dentists to seven days for adults, and five days for minors. Doctors must also provide a specific diagnosis under and procedure code under Kasich’s edict. Physicians who don’t follow the new rules will risk losing their medical license.
Second, Ohio’s two U.S. senators, Bob Hackett of London and Jay Hottinger of Newark, introduced Senate Bill 119, which mandates that all Ohio physicians follow CDC guidelines for treating patients with chronic pain. The bill also mandates both physicians and doctors undergo eight hours of opioid training and make addiction education available online.
Does More Need To Happen?
Walmsley is pleased the state has taken direct action to curb the over-prescribing of opioids, but she sees a lot of room for improvement. Mainly, she sees the need for more aggressive education.
“They install stricter regulations on opioids and then doctors prescribe methadone and suboxone instead. I think education in medical colleges, prior to those people becoming doctors, would help. They need to better understand the impact a prescription can have,” she says.
Walmsley herself was addicted to suboxone at one point. She was on probation from one of her felony convictions and six months sober when she went to see a doctor because she was having trouble sleeping. The doctor prescribed her suboxone and Walmsley thought she had hit pay dirt.
“I was getting so high off it. I thought I had found a way to get high legally while I’m on probation,” she says. “Then it ran out. And it was a worse withdrawal than heroin.”
Working with addicts every day gives her a unique vantage point. She believes suboxone and methadone merely prolong the actual healing process, which requires a person to go without any chemical substance. It’s why she won’t place people who go through the PAARI program into facilities that condone the use of the two drugs.
For Walmsley, everything comes back to education.
She wants medical professionals to be better educated on the dangers of the medications they’re prescribing. She wants greater understanding among the general population about how people become addicts, and she wants education about the dangers of narcotics to start much, much earlier for kids.
“There’s so much education that needs to happen. I was bullied a lot. Did that lead me to smoking weed more often? Did that lead me to this or that? I don’t know,” she says. “It starts young. It starts as early as middle school. People need to be educated early.”
Walmsley had to overdose and nearly die before she had what she almost sarcastically describes as a “spiritual awakening” and finally turned away from all drugs. She’s hopeful that a more cognizant body of medical professionals and a more widely educated population will mean no one else has to almost die to defeat addiction.
Photo from CDC and Patch
Get more local news delivered straight to your inbox. Sign up for free Patch newsletters and alerts.