Health & Fitness
Great Lakes Naval First Responder Credits ‘Telestroke’ With Saving Life
Chad Boeder vows to teach other paramedics first-hand experience of stroke symptoms to help others.
LAKE FOREST, IL — Chad Boeder is a young active paramedic and Emergency Medical Services (EMS) personnel that puts others first before his own needs. However, roles reversed when Boeder went from helping others in medical emergencies to becoming the patient in a medical emergency in a blink of an eye.
Boeder was at work finishing up dinner when he felt an excruciating headache that started from his neck and traveled up to his left temple. Headaches happen often for Boeder who deals with stress, high pressure and long hours as a paramedic at Great Lakes Naval Fire Department and therefore didn’t think anything of it. He decided to take a moment to relax by laying down in his room. Then he started to feel a tingling feeling in his left index finger and thumb as well as a tight feeling in his jaw and that’s when he knew something wasn’t right.
“My first thought was that I was having a heart attack or some sort of heart issue,” said Boeder who resides in Sturtevant, WI. “So I decided to have some of my buddies in the fire department take a look to see what was going on.”
Find out what's happening in Lake Forestfor free with the latest updates from Patch.
Paramedics quickly hooked him up to the electrocardiogram, or EKG, in the ambulance to check his hearts rhythm and found out his symptoms were not due to a heart attack but his blood pressure was through the roof.
He had a family back home – a wife, son and daughter that he didn’t want to leave behind.
Find out what's happening in Lake Forestfor free with the latest updates from Patch.
Boeder tried to shake it off and again headed back to his room to rest off the pain. However he started to feel a severe numbness on his left side of his body and that’s when he knew he couldn’t ignore the symptoms any longer.

His fellow coworkers quickly hooked him up to monitors in the ambulance and rushed him to Northwestern Medicine Lake Forest Hospital. Boeder and other paramedics help stroke patients all the time during the most vital time of a stroke and knew that “time was brain.” They knew that it was essential to get him to the hospital as quickly as possible to save his life. According to the American Stroke Association, a typical patient loses 1.9 million neurons each minute a stroke is untreated which essentially means human nervous tissue rapidly and irretrievably are lost as a stroke progresses. There is usually only a limited window of time to for physicians to be able to administer therapeutic interventions for instance the clot-busting drug, tPa.
“Neuro-Alert! Neuro-Alert! Neuro-Alert” At Lake Forest Hospital, when a stroke patient arrives in the emergency room, a “Neuro-Alert” is activated, triggering a rapid response team to evaluate the patient to ensure that the most appropriate care is provided in the shortest time possible. When Boeder arrived in the emergency room, the rapid response team – including emergency room physicians and nurses – rushed him to imaging to get a CT scan, or computed tomography, which can show if there are abnormalities in the brain. The CT scans are a primary method of determining whether a stroke is ischemic (insufficient blood flow to the brain) or hemorrhagic (ruptured blood vessel hemorrhage) or a different kind of problem. Since Boeder’s stroke was ischemic and signs of his stroke occurred within the three hour timeframe, tissue plasminogen activator, or tPa was given through an IV in his arm to help dissolve the clot and improve blood flow to the part of the brain being deprived of blood flow. tPa may improve the chances of recovering from a stroke drastically.
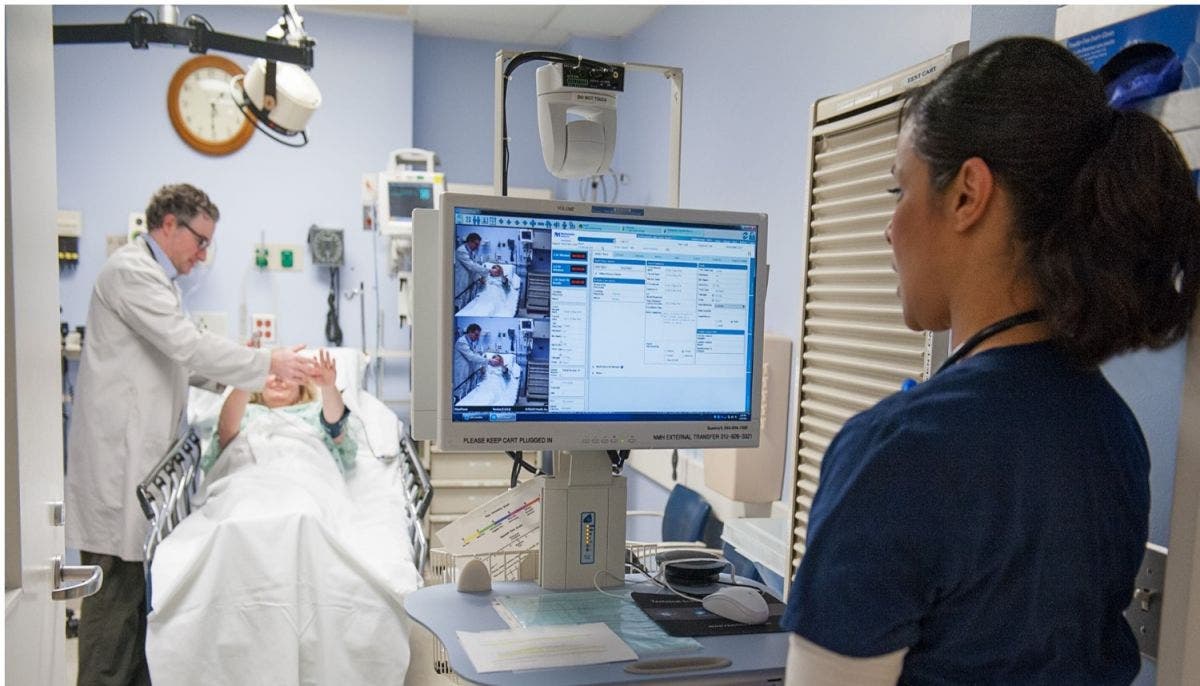
Then Boeder was set up on a video conference using a device called Telestroke which instantly contacts a vascular neurologist expert from Northwestern Memorial Hospital in Chicago to help evaluate a patient, view diagnostic scans and recommend treatment using video conferencing technology and real-time comprehensive patient information.
Leading neurologist on his case and medical director of the stroke program at Lake Forest Hospital said that Telestroke saves lives.
“This program is a huge asset for our stroke program and ensures that our patients receive immediate access to expert neurologic care in the event of a stroke,” said Laura Goldstein, MD, neurologist and medical director of the Northwestern Medicine Lake Forest Hospital stroke program. “Providing Chad with a comprehensive stroke team by utilizing world-class physicians through the Telestroke program, we were able to assess the severity of his stroke and quickly determine the need for acute stroke rescue with an IV tPa.”
To help provide more aggressive stroke treatments, Boeder was transferred to Northwestern Memorial Hospital for further care. He was monitored and evaluated for progress for a few days but didn’t need any surgery or rehabilitation which is remarkable as most patients who have an ischemic stroke from the brain stem have a higher chance of becoming paraplegic.
“I’m thankful I was at the right place at the right time and that Northwestern Medicine was able to take care of me so well,” said Boeder
Boeder went back to work full-time on January 9 and is hoping to start a class lead by him sharing his experience as a stroke survivor as well as helping paramedics better identify and treat patients who are having a stroke.
For more information about Northwestern Lake Forest Hospital’s Wood-Prince Family Stroke Center, visit lfh.org/stroke.
(This post written and submitted by Northwestern Memorial Hospital)
Get more local news delivered straight to your inbox. Sign up for free Patch newsletters and alerts.