Neighbor News
After 200 Years, Technology Improves on the Stethoscope
Scripps Mercy physicians discuss the new look stethoscope for the digital age, a pocket ultrasound device made to look inside the patient.
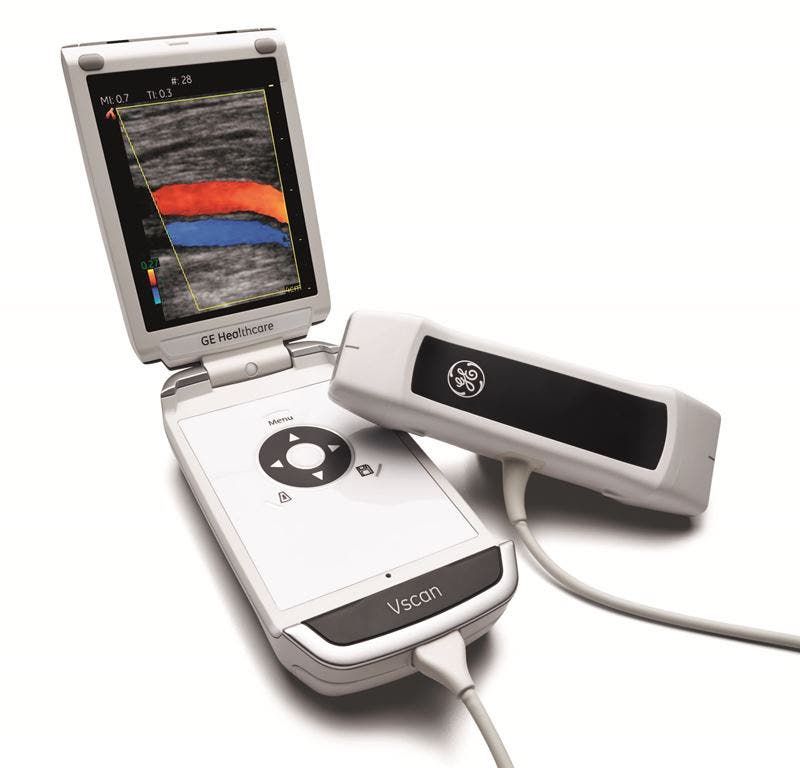
Doctors have been using the stethoscope for the past 200 years to explore the workings of their patients’ heart and lungs. However, this centuries-old technology has significant limitations.
The subtle sounds made by these organs can reveal much about potentially troubling health problems, such an irregular heartbeat, a leaky valve or a buildup of fluid in the lungs. But even the most seasoned physician can have trouble interpreting what he or she hears through this relic of the analog world.
Now, doctors can use a high-tech, digital alternative – a pocket ultrasound device. This innovative piece of technology takes the power of a large ultrasound machine and packs it into portable device that resembles a clam-shell cell phone in both look and size.
Find out what's happening in San Diegofor free with the latest updates from Patch.
“With a pocket ultrasound device, doctors can literally look inside their patients when conducting a routine physician exam,” said Paul Han, M.D., associate director of the Internal Medicine Residency program at Scripps Mercy Hospital San Diego “I can see with my eyes at the bedside in real time how well the heart is pumping or if the lungs are filled full of fluid, instead of surmising it from the ‘lub dub’ or the ‘crackles’ that I may or may not hear in a noisy emergency room.”
But does having an ultrasonic stethoscope necessarily translate into better patient care?
Find out what's happening in San Diegofor free with the latest updates from Patch.
Effort validated by research
Various investigators at Scripps Mercy Hospital, led by Dr. Bruce Kimura, M.D., have been answering this question over the past 15 years and their findings clearly demonstrate the potential power and value of this innovative technology. For instance, in one set of studies, residents were able to detect in patients previously undetected cardiovascular abnormalities resulting in changes to their treatment regimen. In another set of studies, detection of lung abnormalities by this exam was shown to be predictive of poor patient outcomes, suggesting that this technology not only has diagnostic but prognostic utility, as well.
Potential cost-effectiveness has also been addressed by this group, with their studies suggesting that unnecessary expensive diagnostic studies can be avoided based on a normal bedside ultrasound exam. The scope of their investigation also includes learnability and retention of these skills for residents who have undergone this training through the residency program.
Improving quality, lowering costs
Looking at these results in another way, more accurate bedside exams mean that fewer follow-up exams using bigger and more expensive diagnostic devices will be ordered when they actually aren’t needed. Conversely, an unsuspected asymptomatic disease not easily detectable by traditional physical examination may be identified early, resulting in preventative measures against potential medical catastrophe.
“That’s better for the patient, who avoids the time and hassle of more tests,” Dr. Han said. “And it’s good for the health care industry, which is rife with high costs resulting from wasteful and unnecessary practices. Furthermore, the use of this technology is teachable to residents and helps produce more skilled or competent doctors.”
Those are some of the reasons Dr. Han and his colleagues are training the next generation of doctors to use the pocket ultrasound at Scripps Mercy Hospital in San Diego. The Cardiovascular Limited Ultrasound Examination (CLUE) program, which is the first of its kind in the United States, teaches the hospital’s internal medicine residents how to incorporate this device into their routine hospital rounds and clinic visits
As one of the program’s instructors and a former resident who learned how to use a pocket ultrasound through the CLUE program, Dr. Han has seen firsthand the power of this device to make doctors better and, in some cases, to save patients’ lives.
“I’ve also seen how this device can enrich the bond between doctor and patient,” he said. “Our residents can show patients in real time at the bedside exactly what they are seeing on the pocket ultrasound screen and explain what the image means. This is certainly a step in the right direction at a time when more patients want to partner with their doctors to play a more active role in their medical care.”
Right now, the program’s 10 pocket ultrasounds allow 30 residents to conduct more than 7,000 exams with these devices each year.
The Scripps Foundation recently launched a fundraising effort to raise $200,000 for the purchase of 25 more pocket ultrasounds, which would allow each resident to carry a device at all times and greatly increase the number of patients who benefit from the technology.
“To Your Health” is brought to you by the physicians and staff of Scripps. For more information, please visit www.scripps.org/SNS or call (858) 914-2297.