Health & Fitness
North Shore Hospitals Prepare For Influx Of Coronavirus Patients
North suburban hospitals could need to double or even triple their bed capacity to handle cases of COVID-19, according to new data.
EVANSTON, IL — North Shore hospitals will need to expand their capacity to handle the influx of patients projected by even the most optimistic models of the spread of the new coronavirus, according to data from the Harvard Global Health Institute cited Tuesday in a ProPublica report.
The report emphasizes the significance of measures to "flatten the curve" — that is, to reduce the spread of the virus and limit the percentage of the population infected — in order to avoid hospitals becoming overwhelmed with coronavirus patients.
To prepare for the potential surge in patients, health care workers are trying to use supplies efficiently, expand capacity and do "everything humanly and superhumanly possible to keep up and not only provide the best care for patients but keep our staff [safe] as well," according to Dr. Robert Citronberg, director of infectious diseases at Advocate Lutheran General Hospital In Park Ridge.
Find out what's happening in Evanstonfor free with the latest updates from Patch.
"This is not a normal situation. Every day hospitals are assessing their bed situation, supply situation and staff situation to meet the current need in real time," Illinois Hospital Association spokesman Danny Chun said.
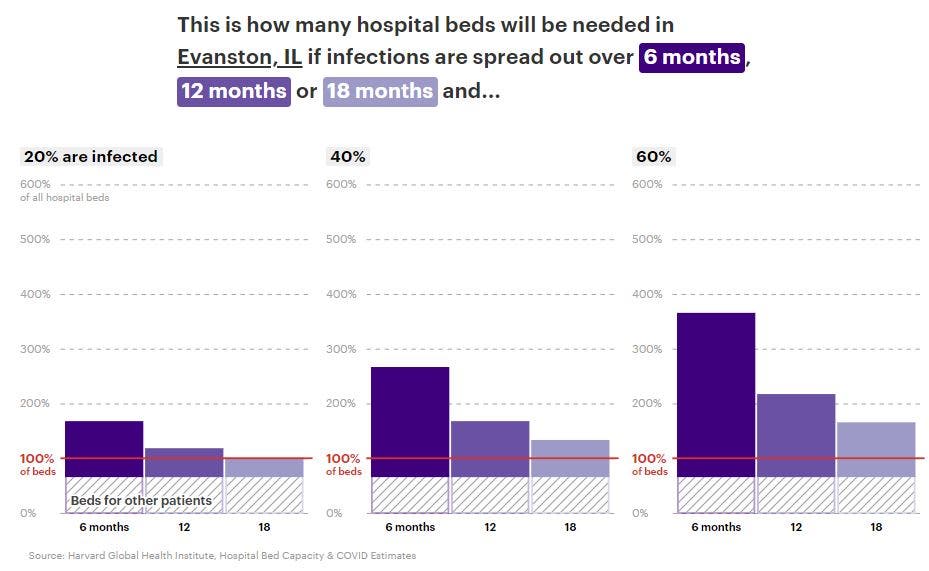
To examine where the need for additional hospital beds would be most acute, researchers considered nine scenarios for how the COVID-19 pandemic might proceed across the United States. They modeled what would happen if 20 percent, 40 percent or 60 percent of adults contracted the novel coronavirus, and whether they caught it over the next six months, 12 months or 18 months.
Find out what's happening in Evanstonfor free with the latest updates from Patch.
The best-case scenario they considered would be limiting coronavirus infections to 20 percent of adults — about 50 million people — and spreading those cases out over the course of the next 18 months. That would bring the number of infections roughly in line with the high-end Centers for Disease Control and Prevention estimate of the number of flu illnesses reported since October.
Hospitals on the North Shore would be only able to meet the demand for beds if the COVID-19 cases were spread out over longer than a year, according to the ProPublica report, which relied on 2018 data. The report does not take into account steps hospitals might take to increase capacity in preparation for an exponential rise in coronavirus cases.
Illinois Coronavirus Update: March 18: Don't miss updates about precautions in the Chicago area as they are announced. Sign up for Patch news alerts and newsletters.
ProPublica reported there were about 670 available beds out of a total of 2,030 in the Evanston "hospital referral region," which extends from the Chicago border to North Chicago and as far west as Palatine, citing data from the American Hospital Association and the American Hospital Directory.
In intensive care units, which are best equipped to handle the most serious respiratory symptoms associated with COVID-19 cases, there were 140 beds available out of a total of 330 in the region.
The region has a population of more than 920,000, with 18 percent over the age of 65. Older adults who contract the novel coronavirus have experienced notably higher rates of hospitalization and death. Using data from China, the Harvard study assumed a fifth of adults who contract the virus will need to be hospitalized for an average stay of 12 days.
In the "moderate scenario" — where 40 percent of adults contract coronavirus over a 12-month period — area hospitals would handle more than 60,000 COVID-19 patients, according to the Harvard Global Health Institute data. ProPublica reported that scenario would require more than 2,000 beds over the next year — three times as many as are normally available — and ICU bed capacity would need to increase to 320 percent of current levels.
Illinois Department of Public Health officials tell Patch they are closely monitoring available resources at hospitals across the state. As of Tuesday, the department reported there were 814 available beds in intensive care units, 597 empty isolation beds and 1,467 ventilators statewide.
A spokesperson for NorthShore University HealthSystem said the company formed an team to plan for the coronavirus in January. it meets daily and reviews supplies, systems, personnel and other aspects of the situation. It has also established new staffing pools to make sure it has enough personnel.
"In addition to our currently designated COVID-19 clinical areas within our hospitals (that include isolation units, negative-pressure patient rooms, etc.), our multidisciplinary team is working on converting additional clinical areas into enhanced COVID-19 isolation units to accommodate a patient surge, should the situation present itself," Colette Urban, NorthShore public relations director, said. "We’re mobilizing clinical and medical personnel from across the organization to provide COVID-19 care and assistance where needed."
NorthShore is also working to maintain its supply of personal protective equipment, like gowns, masks and gloves, according to Urban.
"We are managing our supplies very carefully and sensibly for the protection of our patients and employees, given the worldwide shortages," she said.
Representatives of Northwestern Medicine have yet to respond to inquiries about the ProPublica study, what steps their hospitals are taking to increase capacity or how many beds are available in their intensive care units. Any information they provide will be added here.
Related:
- Hospitals Postpone Elective Surgeries To Prepare For Coronavirus
- How Local Hospitals Are Prepping For COVID-19
- In-House Coronavirus Tests Offered At Evanston Hospital
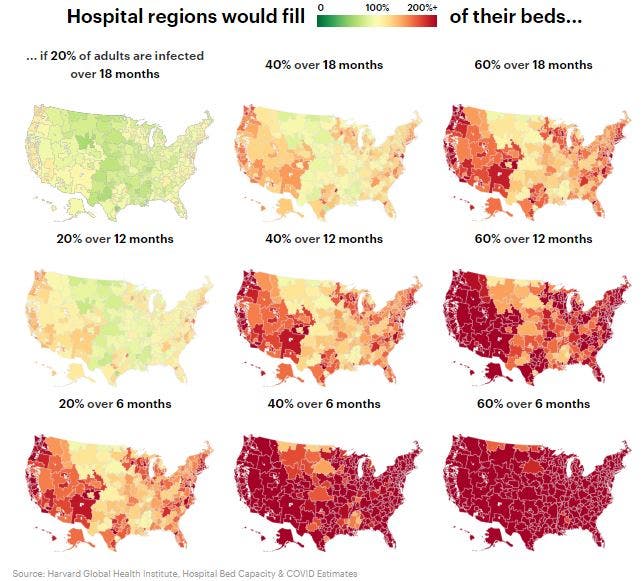
In all but the rosiest scenarios, "vast communities in America are not prepared to take care of the COVID-19 patients showing up," Harvard Global Health Institute Director Dr. Ashish Jha, who led a team of researchers that developed the analysis, told ProPublica.
Hospitals in urban areas are likely to be more stressed, but larger health care systems have more flexibility to shifting patients between locations or discharging them to free up beds, according to the report.
Chicago area hospitals have been taking steps to preserve capacity to prepare to treat an increase in coronavirus patients. Measures have included restricting visitors, rescheduling non-emergency surgeries and limiting outpatient procedures.
"I'm telling my patients to postpone any testing procedures or follow-ups. Don't get a mammogram. Reschedule your colonoscopy. Just wait," Northwestern Medical Center Dr. Kathrine Tynus said. "At the doctor's office we've got people coming in who are sick and worried and the last thing we want to do is expose other patients who are sick and frail in the waiting room."
Patch Partner ProPublica is a nonprofit newsroom that investigates abuses of power and other public concerns.
Read the full report: Are Hospitals Near Me Ready for Coronavirus?
Get more local news delivered straight to your inbox. Sign up for free Patch newsletters and alerts.